
Before laser refractive surgery
First of all, your ophthalmologist will need to examine your eyes fully to determine your suitability to undergo laser surgery. In particular, eye conditions such as keratoconus, dry eye and glaucoma need to be looked for and excluded. It is important to detect beforehand any problems that could potentially affect your outcome after surgery.
The thickness of your cornea (clear window at the front of the eye) will be measured to determine if it is thick enough to undergo refractive surgery. This process is called corneal pachymetry. After that, the curvature of the cornea will be determined with corneal topography. This maps out the cornea and shows which parts are steep and which parts are flat. This scan allows your ophthalmologist to plan how much corneal tissue to remove during your treatment.
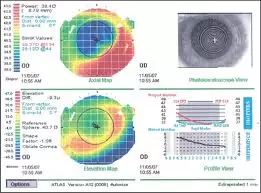
Corneal topography is an essential part of the preoperative evaluation for laser refractive surgery. The results from topography are used to calculate the amount of tissue that needs to be ablated from the corneal stroma.
The new wavefront technology now provides an even more accurate and precise map of visual aberrations that are affecting your vision. This enables your treatment to be customized to the specific requirements of your eye and cornea – ‘custom’ laser refractive surgery. Your cornea will be reshaped to an extremely precise level during the custom procedure. This means that you are even more unlikely to need glasses or contact lenses after laser surgery.
If you wear contact lenses, you must remove your contact lenses to allow your cornea to return to its natural shape. This can take up to 3 weeks, so please check first with your surgeon before your appointment. The corneal measurements must be repeated to make sure that they are stable before you undergo surgery.
During laser refractive surgery
Laser surgery is a relatively quick but delicate procedure that takes up to 15 minutes to perform. You will be asked to lie down for the procedure. Local anesthetic eye drops are usually sufficient to keep your eye comfortable. A clip is placed to keep your eyelids open. Your eye is adjusted so that it is positioned at the correct location under the laser. Your cornea may be marked with an ink marker for orientation during laser.
If you are undergoing a flap procedure, a suction ring will ensure that there will not be inadvertent eye movements that may affect the quality of the flap. The thin, circular corneal flap is created with either a microkeratome blade or a femtosecond laser.
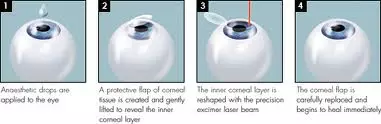
If you are undergoing a surface procedure, the corneal epithelium (‘skin’ over the corneal surface) may either be removed (as in PRK) or lifted and replaced with alcohol and a thin trephine blade (as in LASEK) or just with an epi-keratome blade without alcohol (epi-LASIK).
You will be asked to fix your gaze at a target light during the laser ablation process. It is important that you maintain your fixation to allow the excimer laser to work as accurately as possible as it removes tissue from your cornea. This takes up to 90 seconds.
After laser ablation, the flap is replaced (if you are undergoing a flap procedure). The corneal flap is able to naturally seal itself back into its original position, as though no flap had been made.
Most people feel no pain with laser refractive surgery, although you may still have a slight feeling of pressure during the procedure. You may notice some clicking and whirring sounds during laser. Some people notice an unusual smell during laser. All these are innocuous and will not cause any problems either during or after surgery. No sutures are required.
After laser refractive surgery
Your eye will feel slightly gritty, uncomfortable and light sensitive for the next few days. In some, this may last for a few weeks. This will settle with the antibiotic, anti-inflammatory and lubricant eye drops that you will be given after surgery. You may also be given some special contact lenses to wear for added comfort. Avoid swimming and rubbing your eyes for a few weeks after surgery.
Initially your vision will be blurry. You will usually notice an improvement in your distance vision within a few days. All the laser techniques have very good visual outcomes, with most people achieving a visual acuity of 20/20 (or 6/6) after surgery, especially if performed with wavefront technology. A small proportion of patients may still need spectacles or contact lenses to sharpen up the focus. However, the strength of the spectacle and contact lens prescription will be considerably less than before surgery.
There may be fluctuations in your vision in the first month after surgery. You may also notice haloes around lights, glare and ghosting of images. These should settle should all diminish and stabilize within 3 to 6 months. Even after your vision has stabilized, you should still undergo checks every year to ensure that your eye remains healthy.


You may notice ghosting (top picture) and glare (bottom picture) after surgery. These are usually transient and should gradually improve with time.
As with all forms of surgery, there is always a small risk of complications from surgery. So make sure you know what to expect and always listen to your ophthalmologist regarding any instructions concerning eye drops and caring for your eye after surgery.
Important: As you grow older (especially after 40), your near vision will still deteriorate as part of the aging process presbyopia. Your lens becomes less and less able to change shape to focus at near objects. You will therefore still be likely require reading glasses to improve your near. Laser refractive surgery does not prevent presbyopia. However, just because you have had previous refractive surgery does not mean you cannot have presbyopia treatments to restore your near vision.


