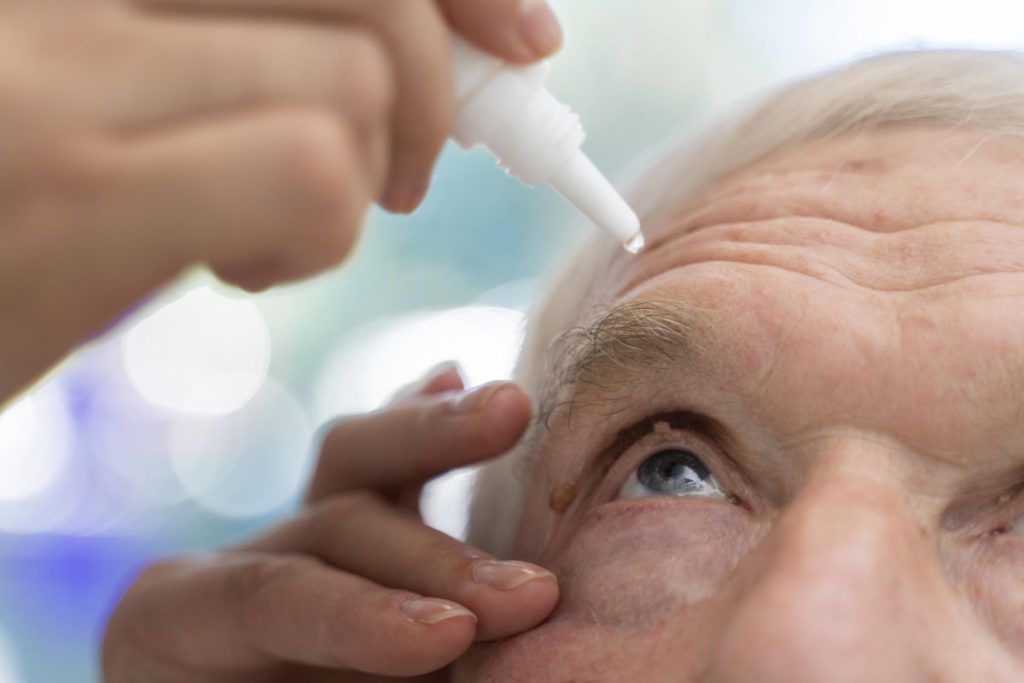
What is glaucoma and why is it important?
Glaucoma is a condition where there is progressive damage to the optic nerve, usually related to high pressure in the eye. This causes visual field loss and if untreated, eventual blindness.
Glaucoma is the second commonest cause of blindness worldwide, and affects at least 2% of the population. It is a major eye health issue, and the most worrying thing is that most sufferers do not know that they have this condition.This is because you usually do not notice any glaucoma symptoms until a lot of glaucoma damage has already occurred.
Unfortunately, glaucoma cannot be ‘cured’ or ‘reversed’, despite the many claims to the contrary that are widespread throughout the internet. Any vision lost from the optic nerve damage cannot be recovered.
The only proven glaucoma treatment option available currently is to reduce the eye pressure, and this can be achieved through eye drops, laser, or surgery.
Please remember that reducing the eye pressure does not restore your vision; it only serves to slow down and reduce the risk of further eyesight deterioration. Hence the focus on monitoring: early detection means early glaucoma treatment and less glaucoma blindness.
The aim of glaucoma treatment is to reduce the eye pressure in order to prevent further worsening of the visual field. The tunnel vision effect from advanced peripheral field loss is well demonstrated in the example above.
I’ve been diagnosed with glaucoma. When should I start treatment and how much pressure reduction do I need?
It makes sense to start treatment for glaucoma as soon as you have been diagnosed. Glaucoma damage is irreversible, so there’s no sense in waiting for more damage to occur first before commencing treatment.
The amount of reduction of eye pressure required depends on how high your initial eye pressure is, and the amount of damage your optic nerve has already sustained. The presence of other risk factors for glaucoma, such as family history and previous eye trauma, also come into consideration.
In general, the normal eye pressure measurements range from 8 to 21 mmHg. In my clinical practice, I will start glaucoma treatment if the pressure consistently exceeds 28 mmHg, even if there is no damage to the optic nerve. I feel that at this level of eye pressure, glaucoma damage is inevitable, so it makes sense to treat pre-emptively before any actual damage has occurred.
However, I will also start glaucoma treatment if there is confirmed glaucoma damage even if the eye pressure is not elevated. This is called low pressure glaucoma.
We know when the eye pressure is reduced, further glaucoma damage to the optic nerve will be less likely and less quick to occur. Unfortunately, there is no specific eye pressure level below which no glaucoma damage will ever happen.
Nevertheless as a general rule, when I start any of my patients on glaucoma treatment, I try to aim for a pressure of 14 mmHg or less.
I am ready to treat my glaucoma. What glaucoma treatment options are there?
The main aim of glaucoma treatment is to reduce the eye pressure. There are 3 ways to do this: with medications, laser, and surgery. The traditional approach is to start with eye drops first, then followed by laser if drops are not effective enough, and then finally surgery as a last resort.
Although medical therapy with eye drops has been considered to be the first line treatment for glaucoma, there is now increasing evidence (including from the international multi-center, randomized clinical trial that I was the lead author on) that laser treatment can also be an effective and equivalent first line treatment.
Having said that, medications (eye drops and oral) remain the commonest form of glaucoma treatment worldwide, and works well in the great majority of patients. In this section, I discuss the medications used for glaucoma treatment.
Glaucoma treatment with eye drops
Eye drops for glaucoma usually act in one of two ways. They ‘turn off the tap’ by reducing the production of aqueous (natural fluid in the eye) from the ciliary body. Alternatively, they ‘improve drainage’ by increasing the outflow of aqueous from the eye via the existing drainage channels.
Sometimes the pressure-lowering effect from a single medication is not enough. It is common to need to use combination of multiple eye drops to achieve the desired pressure. Sometimes you may also need laser treatment or surgery, in addition to your eye drops, to achieve the target pressure set for your eyes.
There are 5 main classes of pressure lowering eye drops: prostaglandins, beta blockers, alpha agonists, carbonic anhydrase inhibitors, and pilocarpine.
Prostaglandin eye drops encourage the drainage of aqueous from the eye. They are usually instilled once daily at night, and are very effective and safe. Prostaglandins are the first line eye drop treatment for glaucoma. Eye drops in this class of medication include latanoprost, bimatoprost, travoprost and tafluprost.
The commonest side effects of prostaglandins include the elongation and darkening of eyelashes, darkening of the skin around the eyes, and irritation of the eyes.

The eyelashes can grow significantly longer when prostaglandin eye drops are used for prolonged periods. Once the medication is stopped, the eyelashes will eventually return to their original length. Many eyelash-enhancing serums contain prostaglandin to increase eyelash length. These include Latisse (which contains bimatoprost), RevitaLash and GrandeLASH.
Beta blockers reduce the production of aqueous from the ciliary body. They are usually administered twice daily. Some long acting preparations allow once daily instillation. Until the introduction of prostaglandins, beta blockers were the first line eye drops for glaucoma. Examples of beta blocker eye drops include timolol, carteolol, levobunolol, metopranolol and betaxolol.
The main side effect of concern is shortness of breath. So if you have asthma, you should not take beta blocker eye drops. In the elderly, beta blockers may cause a slowing of the heartbeat, low blood pressure and lightheadedness. Other potential side effects include eye irritation, fatigue and hair loss.
One unique feature of timolol is that it can be combined with the other medication classes to form a combination eye drop in a single bottle. Timolol can be combined with prostaglandins (latanoprost-timolol, travoprost-timolol, bimatoprost-timolol, tafluprost-timolol), alpha-agonists (brimonidine-timolol), and carbonic anhydrase inhibitors (brinzolamide-timolol and dorzolamide-timolol).
Alpha agonists work by reducing the production of aqueous, and also by to encouraging aqueous drainage. They are usually instilled either twice or 3 times daily. Examples of alpha agonist eye drops include brimonidine and apraclonidine.
The commonest side effect is redness and irritation of the eye. This occurs in around 15% of the time. Alpha agonists should also be used with caution in children under 5 years due to possible depression of the respiratory and central nervous systems.
An added benefit of treatment with brimonidine is that it may also provide additional protection to the optic nerve, although the scientific evidence for this still requires further support.
Carbonic anhydrase inhibitors act by decreasing the amount of aqueous produced by the ciliary body. They are usually administered twice or 3 times daily. Examples of carbonic anhydrase inhibitor eye drops include dorzolamide and brinzolamide.
The commonest side effects are bitter taste in the mouth after instillation and irritation of the eye. Carbonic anhydrase inhibitors are the least effective among all the eye drops in decreasing eye pressure.
Brinzolamide can be combined with brimonidine to form a brinzolamide-brimonidine combination eye drop in a single bottle.
Pilocarpine is the oldest and least used of all the glaucoma eye drops. It acts by increasing aqueous outflow from the eye and constricting the pupil so the anterior chamber drainage angle becomes widened. It is used most commonly for angle closure.
Side effects include significant headache, brow ache and blurred vision at night. These side effects can be quite unpleasant.
Pilocarpine is generally no longer used for open angle glaucoma because it is poorly tolerated and prolonged treatment causes persistent small pupils which makes clinical examination of the back of the eye difficult.
I’m using glaucoma eye drops but I’m confused because my doctor now wants me to change to a different drop.
Sometimes your glaucoma treatment with eye drops needs to be changed.
One reason is that the current drops that you are using do not lower your eye pressure enough. In this case, the eye drops are simply replaced with a different one, or new drops are added to the ones that you are currently already using.
Another reason is that they are causing side effects (see above) or an allergic-type reaction that you are not able to tolerate.
In eye drop allergy, your eyes will sting (a lot!) with each instillation of the eye drop, and may persist for a few minutes after that. Your eyes and eyelids will also become very red, irritable, and weepy. If these symptoms occur, please do not persist and bear with the drops. Just stop them immediately.
If you experience any difficulties or problems with the eye drops, you must let your ophthalmologist know as soon as possible. The important thing is to get you on effective treatment for your glaucoma with as little side effects as possible.
Do you have any useful tips about using glaucoma eye drops?
I get this question a lot from my patients.
It goes without saying that you should use your glaucoma eye drops daily as instructed by your eye specialist. The only reason you should stop using drops on your own accord is if you are starting to develop an allergic reaction or intolerance to the eye drops.
I have listed 5 useful tips that will make using eye drops a smooth and easy, yet effective process.
Tip #1: More is better than less
It’s not always possible to be 100% accurate with instilling eye drops. Sometimes the drop just ends up on your eyelid, and sometimes on your cheek. Sometimes even if the drops aren’t on your eyelid or cheek, you just can’t tell if the medication has entered your eye or not.
If you are not sure whether the drop has gone in the eye, then try again. There is no harm in putting an extra drop or two if you’re unsure. In this situation, more is better than less.
Tip #2: Press on your tear ducts (punctal occlusion)
After you have put the drops in your eyes, you should press on your tear ducts located in the inner corner of your eye. Do this for around 1 minute (2 minutes if possible).
Also keep your eye shut and try not to blink during this time.
By doing this, you block your tear ducts from draining out the drops too quickly. This maximizes the absorption of the medication into the eyeball and optimizes its pressure-lowering effect.
The picture below shows an example of punctal occlusion.

Tip #3: Leave 5 to 10 minutes between different drops
It is very common for your glaucoma treatment to involve multiple types of eye drops in different bottles.
If you are instilling different drops at around the same time, it doesn’t matter which drops go in first. What matters is to make sure that they go in at least 5 to 10 minutes apart.
Doing this maximizes the absorption of the individual eye drops into the eye.
Tip #4: Eye drop aids
The eye drops are contained within plastic bottles which can sometimes be difficult to squeeze.
Most bottles can be used with eye drop aids that make the bottles easier to handle. This is very helpful in the elderly and in those with hand weakness or hand movement difficulties, such as in rheumatoid arthritis and Parkinson’s disease.
Below are a selection of useful eye drop aids that are available for purchase through Amazon:
Tip #5: Preservative-free eye drops
It is now well-recognized that preservatives in eye drops (such as benzalkonium) can cause eye irritation. Preservatives are important because they prevent microorganisms from growing in the liquid medication contained within the eye drop bottle.
The chemicals contained in the preservatives are similar to what you might find in laundry detergent. So you can imagine the kind of irritation your eye might experience if you were to put laundry detergent a few times a day into your eye. The irritation is made much, much worse if you have dry eye disease.
There are now preservative-free or preservative-minimal preparations for most of the glaucoma eye drops. Please discuss this with your eye specialist if you wish to use preservative-free eye drops for your glaucoma treatment.
Glaucoma treatment with oral medications
There is only one class of oral medication that is prescribed as glaucoma treatment to reduce the eye pressure: carbonic anhydrase inhibitors. They work by decreasing the amount of aqueous produced by the ciliary body.
There are 2 types of tablets in this class of medication: acetazolamide (Diamox) and methazolamide. They are usually taken with food 3 to 4 times daily. Acetazolamide is the more potent of the 2, with better pressure lowering effect but also more side effects.
Acetazolamide and methazolamide are usually prescribed when the eye pressure remains too high despite maximal treatment with all the possible eye drops.
The most common side effects include tingling of the hands and feet, tiredness, stomach upset, and having to go to the toilet more often to pass urine. More serious side effects include kidney stones, low blood potassium levels, and kidney failure.
Due to the seriousness of some of these side effects, Diamox is not ideal for long-term use. It is considered usually as a short-term measure to control the eye pressure until surgery can be performed.
No surprises then that you will need to be closely supervised by your specialist and family doctor if you are being started on treatment with oral Diamox.
I’ve been started on oral diamox because my pressures are too high. Are there any special precautions I need to take?
Diamox is not a pleasant medication to take. It has plenty of side effects, some less serious but others more so. The only reason why you might have to take it is because there is no other medication that can reduce the eye pressure as effectively as Diamox.
In my own clinical observations, most patients are able to tolerate a short course of oral Diamox. However, I’ve known of some patients who have had to be rushed to the Emergency Department due to severe side effects.
Here I list 3 important tips to reduce your risk of developing complications from taking oral Diamox.
Tip #1: Drink plenty of fluids
Diamox is a diuretic, meaning it makes you urinate more. You are more likely to become dehydrated and to develop kidney stones and kidney failure. By drinking plenty of fluids (and by fluids, I mean water), you remain well-hydrated and reduce your risk of kidney problems.
Tip #2: Eat bananas
Diamox can cause low potassium levels in your body (hypokalemia). Hypokalemia is bad news because it can cause your heartbeat to go all haywire. To reduce your risk of hypokalemia, you can eat more bananas, which are a rich source of natural potassium.
Tip #3: Regular blood tests
If you have to take Diamox on a long-term basis, you will need to undergo regular blood tests, every 1 to 3 months. This is to test for electrolyte imbalances in your blood, which is a good indicator of how well your kidneys are coping with Diamox.
Final word on glaucoma treatment with medications
Follow the instructions as given by your eye specialist. The medications are only effective so long as you are using them. So try to set a routine that means you’ll remember to take your medications daily at the set times. This is a long-term game and you need to set yourself up for success.
The only time you can stop using the medications is if you experience side effects that you are concerned about. If these occur, please contact your eye specialist without delay.
See Related: The six best glaucoma supplements for your optic nerve





