The COVID-19 pandemic has brought many changes to our day to day lives. This includes changes to how healthcare services are currently operating. These changes also affect eye care and eye health services.
You may have experienced cancelled appointments, postponed operations and delayed scan; and you may be wondering why.
Possible changes to eye care services
Eye health care services involve some of the most vulnerable people in society including the elderly and those with diabetes. Therefore, the service has been adapted to ensure the safety of all patients and staff.
● Reduced face-to-face appointments. There is a new emphasis on conducting telephone/video consultations (tele-consults) where possible to reduce unnecessary exposure. If there is a clinical need to have a face-to-face appointment, then this can be arranged by the clinician involved. You may be asked to have scans before speaking to an ophthalmologist. These scans may take place in a unit/building which is new to you.
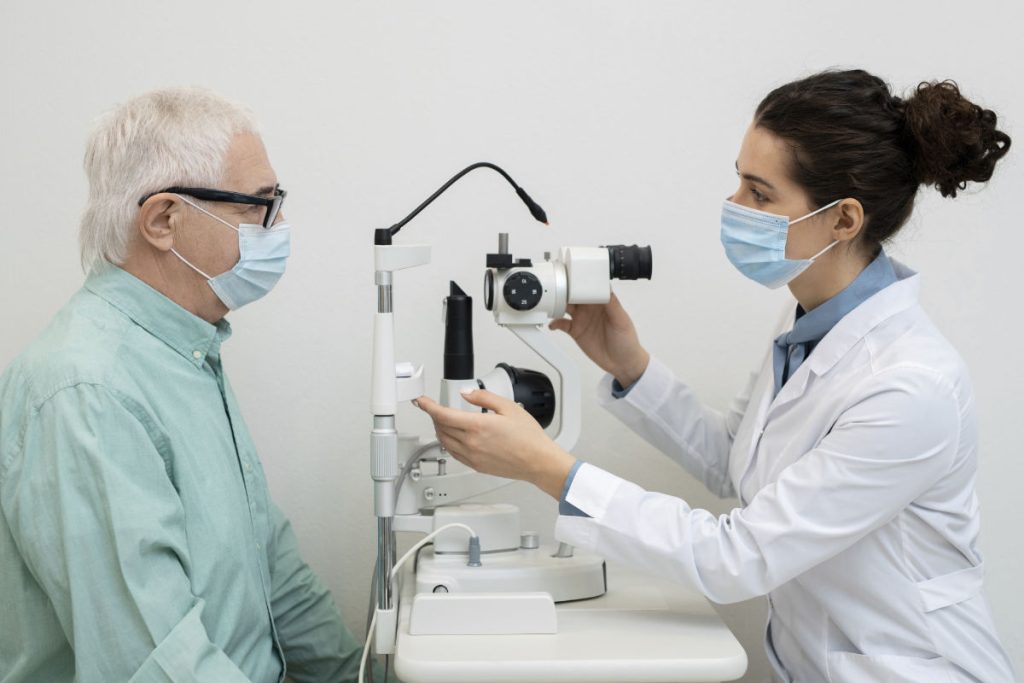
● If you attend for a face-to-face appointment, you will be asked to wear a face covering and you will notice your clinician will also be wearing one. You may be asked to wait in your car or sit apart from others in a waiting room until your appointment time. You may be asked to attend your appointments alone where possible. You may notice that there is a plastic shield or covering placed on the slit lamp used for examinations.
● There may be a preference to perform surgery with local anesthetic instead of general anesthetic where possible. You may be asked to take a COVID-19 swab and to self-isolate before your operation.
● Encouragement of use of other eye health services such as your local optometrist or your family doctor.
● Postponing non-emergency surgery such as cataract surgery. This will lead to increased waiting time for elective surgeries.
● You may be required to demonstrate a negative test on rapid antigen or PCR testing before a laser or surgical procedure.
Please remember that the changes made to eye health services are to protect patients and staff from COVID-19. Please try to be patient with staff during these difficult times.

Social distancing and wearing of masks in hospitals and clinics help to prevent the spread of COVID-19 to the elderly and those vulnerable to infections.
When to seek emergency eye care
Due to these changes, there is likely to be a delay in seeing an ophthalmologist as part of your routine eye health care. However, most emergency eye care services are still running. It is therefore important that you seek urgent medical attention should you notice any of the following:
● You have noticed loss of vision.
● You have a severe headache, eye pain, reduced vision, and feel sick. This combination of symptoms may indicate acute angle closure glaucoma.
● You have noticed changes to your vision, such as flashing lights (which may indicate retinal detachment) and distortion or wavy lines (which may indicate macular degeneration).
● It is painful to look at light. Sensitivity to light is a sign of uveitis.
● You have injured or pierced your eye. Most eye trauma will heal with eye drops, but severe injuries may require emergency surgery.
● A foreign body is stuck in your eye (such as a piece of glass or grit).
It is important to only attend the emergency department if there is a medical emergency. Some countries, such as the United Kingdom, have a helpline you can call if you are unsure whether or not you need urgent medical attention.
You may be asked further questions about your health before speaking to a doctor. The doctor may ask for a video call, come to see you in person or ask you to attend the emergency department depending on their assessment.
Please note that the information above is a general guide only. Regulations and rules may vary from country to country, and even region to region within the same country. The best option is to contact your local eye care service for further information.


